I have been mulling over writing this blog piece for well over a month, never having it quite crystallize. I read a piece in one of my favorite blogs, The Incidental Economist today which served to prompt me to put fingers to keyboard...(http://theincidentaleconomist.com/wordpress/another-hospital-stay-and-whats-not-being-discussed-in-a-polarized-health-policy-debate/).
I live and function in this dysfunctional world. There are lots of very smart and caring people but smart and caring does not trump bad process and bad incentives. The individual problems associated with care of specific patients are often very complex, but the shared problems across many patients are remarkably simple. We have moved to a team based approach to care, particularly in patients with complex and chronic problems, but there is no team leader. This is evident with nearly 100% of the patients I see. All new patients who I evaluate I ask, "Who is in charge?" The answer is invariably, "I don't know."
Sometimes a particularly assertive physician will assume this role but this is the exception rather than the rule. In the inpatient setting, the move toward hospitalists has created a very short term outlook when it comes to management of patients. They head a team of providers whose job is to get the patient discharged as soon as possible. Don't get me wrong. Many of my hospitalist colleagues are wonderful physicians and if placed within a system which gave them the tools and incentives to consistently do more and extend their impact beyond the hospital stay, they would do so.
Some efforts are being made to do just that in order to avoid readmissions. It is in this realm that these efforts are running into the fundamental problem. Even if the hospital coordination and team creation issue is addressed, when a patient is discharged there is no consistent hand off infrastructure present which leads to a soft landing. When sick patients leave the hospital, who is in charge, what resources do they have at their disposal to address the problems they face, and how well prepared are they to address the problems they will face?
Even without hospitalizations, distributed management of multiple problems facing patients is an iffy proposition at best. We can view various roles in the care of an individual patient much like the roles played by various subcontractors when a building project is undertaken. In order to build a house you need carpenters, plumbers, electricians, roofers, heating air specialists, architects, landscapers, and engineers (and I could go on and on). While some people are ambitious enough to take on functioning as their own general contractors, most of us are willing to pay to delegate that responsibility to someone who we trust will coordinate the activities of all of these subcontractors and look out for your interests. It can and should be money well spent.
We face a similar situation in medicine with instead of plumbers and electricians, we have urologists and neurologists and we have one other major difference. We do not have medical general contractors. Perhaps at one point general internists, family practitioners, and pediatrician filled these roles, but as a rule they do not anymore. As we have moved to more specialization and complexity, we have become more silo'd and fragmented. We are trying to undertake major building and renovation projects with our bodies without the benefit having someone who knows what they are doing in charge. Better information systems and communication are necessary but they are not sufficient. A leader need to be charged with synthesizing the information and addressing the big picture with individual patients.
In almost any other realm of the economy this niche would have been filled with resourceful individuals who see a need and create a service to fill that need. However, in health care the payment system created barriers to responding to this need. First, insurance created the impression that health care services were covered and patients assumed that when they became sick, these sort of services were available through their regular providers. Second, those in the best position to provide these sort of coordination services are ones who have undergone extensive medical training. They have had little incentive to take risks and provide services which are not covered by insurance. Finally, the issues with the present state are even more nuanced since patients assume that this sort of service is already built into the health care system and doctors are reticent to explicitly admit they do not consistently provide them. I suspect that many physicians are reticent to admit this to themselves.
The concierge movement is addressing at least some of these concerns. It is a recognition that certain physician activities (and perhaps this should not be limited to doctors) are not compensated by traditional insurance and like other non-insured activities such as cosmetic surgery, providers should be able to seek payment directly from patients. This concept generates strong opinions with accusations that seeking such fees is immoral. I have a hard time seeing the logic. Patients need professionals who function as leaders of the teams who manage their medical problems. To create a world where those individuals don't exist is to guarantee that patients will be left holding the bag.
Definitely not a follower: Following the herd will get you to where the herd is going
Sunday, August 26, 2012
Tuesday, August 14, 2012
Vagueness in medical practice
When it comes to medical deliverables, things often get vague. I came across the following story written in a column by the NYT health reporter Tara Parker-Pope which illustrates this well. She recounts an unhappy series of encounters with the health care delivery system relating to her daughter's ankle sprain. (http://well.blogs.nytimes.com/2012/07/25/too-much-medical-care/?smid=tw-share) She describes that after her daughter sprained her ankle, they embarked upon a six month ordeal attempting to address her daughter's painful ankle. After growing impatient with the pediatrician's wait and see attitude, they saw a series of specialists, each doing a cursory exam, ordering lab and imaging studies. After five months they appeared to be getting nowhere. She wrote:
While this reporter had years of experience in the health care realm and considered herself a well informed patient, she appears to have missed the obvious. What were her goals in taking her daughter to the doctor in the first place? What particular service was she expecting to receive and what deliverables did she anticipate to have delivered? Ultimately, they focused on pain relief and the problem resolved. I have to wonder what were they focusing on prior to that?After years of reporting on health, I considered myself a well-informed patient, but it took my elementary-school daughter to state the obvious: She was the victim of too much medicine. Every new blood test, scan or X-ray raised new questions, which led to more lab work, scans and X-rays. I know the doctors had good intentions, but it’s a truism of modern medicine that the more you test and scan and look for problems, the more likely you are to find something wrong. My daughter’s case had spiraled out of control.I canceled all her appointments with the various specialists, and went back to the sports doctor. We discussed a new approach that focused solely on pain relief. He consulted with my daughter’s pediatrician, and they agreed on a treatment. Within days, my daughter’s ankle had stopped throbbing, and soon she was back to sports and dancing.
While I am not a fan of the PPACA, I think the PCORI element has gotten the patient empowerment conceptually right. If every patient approached their encounters with the health care industry based upon these principles, it would help avoid such stories as described in Mrs. Parker-Pope.
Patient-Centered Outcomes Research (PCOR) helps people and their caregivers communicate and make informed health care decisions, allowing their voices to be heard in assessing the value of health care options. This research answers patient-centered questions such as:
- “Given my personal characteristics, conditions and preferences, what should I expect will happen to me?”
- “What are my options and what are the potential benefits and harms of those options?”
- “What can I do to improve the outcomes that are most important to me?”
- “How can clinicians and the care delivery systems they work in help me make the best decisions about my health and healthcare?”
The cost of this ankle injury had reached well into the thousands of dollars — I had lost track because it was all covered by my insurance.How illuminating. Insulating patients for financial impact tends to make them less reflective about their decision. When the tests were ordered during the specialist visits, were the ordering physicians queried as the potential benefits and harms and the likelihoods benefits of each study, particularly the third MRI? What on earth were they looking for, particularly when they were assuming that whatever it is was it was missed by the previous evaluations? What were the anticipated deliverables from these specific tests and how would that have changed treatment? In an ideal world and equipped with the right questions and expectations, they would have ended up in the same place with fewer tests and visits. Perhaps if they required investment fo their own resources they would be more inclined to think about the PCORI questions.
At some point the patient deliverables diverged from the physician deliverables. Visits to the rheumatologist and ophthalmologist clearly indicated that the their interests had moved away from the painful ankle, suspecting some sort of systemic problem extending beyond the ankle sprain. Perhaps reasonable enough but placed within this context, it behooves the patient (or her mother) to ask the simple question, "How likely is that to be the case?". We are not talking about exact numbers here but decisions to embark on such diagnostic wild goose chases should be supported by knowing whether likelihoods are in the ranges of 1:100 or 1:100 million. In the mean time what are we to do about the ankle which is still painful.
Ultimately, the road to daylight needs to be patient driven. For patients, have a plan in mind when you come to see us. We will make up our own deliverables if you do not articulate them to us first. Are you coming to medical provider because you have an immediate and symptomatic problem (short of breath, pain, inability to function as normal) or are you coming to be reassured that you will be OK in the future? Vague requests tend to prompt vague courses of action. If you are clear about your agenda, be suspicious when your doctor changes it to a different agenda.
Don't settle for just a diagnosis. Ask what this means for you. A diagnosis is simply a prediction. Ask for what that prediction is and the likelihood of specific outcomes. Be aggressive when inquiring as why specific decisions are recommended. Ask for specific numbers and don't settle for terms such as common or rare. They are vague terms. They may mean something to your physician and something entirely different to you. In the same vein, while rejecting vague terms, be prepare to accept uncertainty and admission that we do not know.
Wants and needs and menus
What health care delivery shares with many other industries is it addresses human wants and needs and for the most part it delivers care directly to end users, the patients. To understand how to accomplish various health care related tasks better, perhaps we need to look at a most fundamental question? What does it take to address human wants and needs? In some contexts it is very simple to address this. A person drives up to a window at a fast food restaurant at lunch time and they are hungry. They order a sandwich and a drink off of the menu. They want it hot, fast, and tasty. The rules of the game are that you need to order from the menu. You generally cannot order food from your car where there is no drive through (although you can call in using your cell phone). You also cannot get food in a drive through laundry or drop off your laundry at the McDonald's drive through. Virtually everyone understands these rules unless you are Borat.
 However, not all circumstances are so easily addressed. In particular, the health care industry does not provide such clear signals as the fast food industry as to where clients needs to go in order to get their needs and wants addressed. Health care services are generally offered without menus. There are exceptions to this rule. The retail clinics post their menus and their prices. This does not stop patients from trying to order off the menu, looking for a convenient place to seek help for acute chest pain, acute fractures, or anaphylaxis. We try to inform people what is clearly off the menu. If I call my physician (of virtually any sort), the first thing I hear is the opening message of the phone tree. It tells me that if I have an acute and life threatening problem I should hang up the phone and call 911. That is simply not on the menu of services offered and that is made clear right up front. It is one of the only things made clear in terms of services offered or encouraged.
However, not all circumstances are so easily addressed. In particular, the health care industry does not provide such clear signals as the fast food industry as to where clients needs to go in order to get their needs and wants addressed. Health care services are generally offered without menus. There are exceptions to this rule. The retail clinics post their menus and their prices. This does not stop patients from trying to order off the menu, looking for a convenient place to seek help for acute chest pain, acute fractures, or anaphylaxis. We try to inform people what is clearly off the menu. If I call my physician (of virtually any sort), the first thing I hear is the opening message of the phone tree. It tells me that if I have an acute and life threatening problem I should hang up the phone and call 911. That is simply not on the menu of services offered and that is made clear right up front. It is one of the only things made clear in terms of services offered or encouraged.
Once a patient has gotten past the filter directing them to 911, there are few clues as to where to go. Retail clinics have identified a list of twenty or so services which can be managed in a relatively rules based manner. They represent the fast food equivalent although the discounts offered are more in the realm of time than money. There are a host of services advertised aggressively in assorted media outlets where menus are well defined. These tend to be value added processes and also represent either non-insured procedures or ones where the margins are sufficiently high and competition exists to deliver. No long term commitment here. These are practices looking for people to do things to, drop a bill, and after the value is added (or not) be in search of new game. In the cash business, the price mechanism operates but in the insured realm price controls keep the prices from falling.
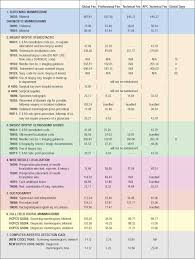 There is a master menu of covered medical services but the public is not really aware of its presence. There are rarely defined prices linked. It is called the CPT (Current Procedural Terminology) code book. It is owned by the AMA which makes a handsome sum of money licensing these. At first it appears there are a dizzying number of codes, over 7500, corresponding to some medical service which gets charged. The numbers may seem large but let's compare restaurant menus to medical menus.
There is a master menu of covered medical services but the public is not really aware of its presence. There are rarely defined prices linked. It is called the CPT (Current Procedural Terminology) code book. It is owned by the AMA which makes a handsome sum of money licensing these. At first it appears there are a dizzying number of codes, over 7500, corresponding to some medical service which gets charged. The numbers may seem large but let's compare restaurant menus to medical menus.
The CPT codes have changed only modestly over the past 30 years. There are new ones approved but the lion's share of codes in existence now were the same as when I trained long ago. Compare that to the food and restaurant business. Think of all of the cuisines which essentially unheard of in this country 30 years ago. The menus of the food business have exploded. We have new cuisines and expansion of old cuisines. In contrast, the menus of the health care field has stagnated. Everybody uses the same ones. The prices are set administratively. We have access to new high profile drugs and high tech equipment but the ability of the industry to better address individual patient wants and needs has gone essentially nowhere.Review the process to get codes added or changed and you can see why.
CPT is a menu which is not for patients, but for those providing the services. The reality is there are no readily accessible menus for patients because the options developed are not about what patients want. They focus on what the experts believe that patient need, a perception strongly influenced by the financial interests of those vested in the current system. Patient choice and empowerment may sound good but they are not really on the table. Create an environment to reward patients who control their own resources and menus with prices will come quickly. So will new menu offerings.
Once a patient has gotten past the filter directing them to 911, there are few clues as to where to go. Retail clinics have identified a list of twenty or so services which can be managed in a relatively rules based manner. They represent the fast food equivalent although the discounts offered are more in the realm of time than money. There are a host of services advertised aggressively in assorted media outlets where menus are well defined. These tend to be value added processes and also represent either non-insured procedures or ones where the margins are sufficiently high and competition exists to deliver. No long term commitment here. These are practices looking for people to do things to, drop a bill, and after the value is added (or not) be in search of new game. In the cash business, the price mechanism operates but in the insured realm price controls keep the prices from falling.
The CPT codes have changed only modestly over the past 30 years. There are new ones approved but the lion's share of codes in existence now were the same as when I trained long ago. Compare that to the food and restaurant business. Think of all of the cuisines which essentially unheard of in this country 30 years ago. The menus of the food business have exploded. We have new cuisines and expansion of old cuisines. In contrast, the menus of the health care field has stagnated. Everybody uses the same ones. The prices are set administratively. We have access to new high profile drugs and high tech equipment but the ability of the industry to better address individual patient wants and needs has gone essentially nowhere.Review the process to get codes added or changed and you can see why.
In Atlanta alone there are almost 400 restaurants listed on Open Table alone. That is a fraction of all the restaurants in this city. If each had only 20 items on their menu, that alone would match the entirety of the options in the entire CPT code book. Consider if each of these restaurants were limited in terms of their menu offerings to only what was approved in say we call it the CCO code book (Current Cullinary Offerings). Want to create a new pizza at Fellini's. You will need a new CCO code. After review by all of the cullinary experts and other stakeholders, we are forced to address the question as to whether the public really needs a new pizza variety? The experts say no. There are enough food choices to address public needs. Who cares about what they might want. That is not important. We we should probably cut back on choices since the public is getting too fat.How are requests for changes to CPT reviewed?Specific procedures exist for addressing requests to revise CPT, such as adding or deleting a code, or modifying existing nomenclature.Medical specialty societies, individual physicians, hospitals, third-party payers and other interested parties may submit applications for changes to CPT for consideration by the Editorial Panel. The AMA’s CPT staff reviews all requests to revise CPT including applications for new and revised codes. If AMA staff determines that the Panel has already addressed the question, staff informs the requestor of the Panel's coding recommendation. However, if staff determines that the request presents a new issue or significant new information on an item that the Panel reviewed previously, the application is referred to members of the CPT Advisory Committee for evaluation and commentary. Applications that have not received any CPT Advisor support will be presented to the CPT Editorial Panel for discussion and possible decision unless withdrawn by the applicant. Applicants will be notified if their applications have received no CPT Advisor support approximately 14 days prior to each meeting of the CPT Editorial Panel meeting. Applicants have the ability to withdraw their applications up until the agenda item is called at the meeting—thereafter the CPT Editorial Panel has jurisdiction over the agenda item.The CPT Editorial Panel meets three times each year. AMA staff prepares agenda materials for each CPT Editorial Panel meeting. Panel members receive agenda material at least 30 days in advance of each meeting, allowing them time to review the material, review CPT Advisor comments and confer with experts on each subject, as appropriate. The Panel addresses nearly 350 major topics a year, which typically involve more than 3,000 votes on individual items.A multi-step process naturally means that deadlines are very important. The deadlines for submitting code change applications and for compilation of CPT Advisors’ comments are based on a schedule which allows at least three months of preparation and processing time before the issue is ready for review by the CPT Editorial Panel. The initial step, which includes AMA staff and CPT Advisor review, is completed when all appropriate CPT Advisors have been contacted and have responded, and all information requested of an applicant has been provided to AMA staff.Following review and compilation of CPT Advisors’ comments, AMA staff prepares an agenda item that includes the application, compiled CPT Advisor comments and a ballot for decision by the CPT Editorial Panel. Once the Panel has taken an action and preliminarily approved the minutes of the meeting, AMA staff informs the applicant of the outcome.The Panel actions on an agenda item can result in one of four outcomes:
- addition of a new code or revision of existing nomenclature, in which case the change would appear in a forthcoming volume of CPT;
- referral to a workgroup for further study;
- postponement to a future meeting (to allow submittal of additional information in a new application); or
- rejection of the item.
Applicants or other interested parties who wish to seek reconsideration of the Panel's decision should refer to theprocess described on the AMA/CPT website.
CPT is a menu which is not for patients, but for those providing the services. The reality is there are no readily accessible menus for patients because the options developed are not about what patients want. They focus on what the experts believe that patient need, a perception strongly influenced by the financial interests of those vested in the current system. Patient choice and empowerment may sound good but they are not really on the table. Create an environment to reward patients who control their own resources and menus with prices will come quickly. So will new menu offerings.
Thursday, August 9, 2012
Health care economics and the "fatal conceit"
I have to give the authors of the NEJM commentary credit. They have succeeded in taking unguarded optimism to new heights. They conceive of and attempt to design an entirely new world of health care economics, all using 3500 words or less. Never short on confidence, they do not let minor operational details get in the way of some good sounding ideas. I selected key elements of this article for comment and have edited out sections for brevity. I believe that the message from the authors has not been substantially altered. The entire article is available at http://www.nejm.org/doi/full/10.1056/NEJMsb1205901.
Everyone (or at least almost everyone) agrees that we have a problem in health care. We are going broke because of costs. We have millions of uninsured. We have millions of under insured. We have problems with access to care, even among the ranks of the insured. We have problems with quality and safety. Have no fear, this elite group of very bright people can rebuild and rewire the house of medicine, even without having to turn the power off. There is a small problem, however. It appears as thought they haven't a clue as to how they can actually accomplish this these tasks. Take for example their first charge:
But there is more...
 That's the ticket! An independent council. Now all of our problems are solved. All we need to figure out how the members of this council could remain independent (of what?), avoid issues of regulatory capture, and be able to avoid the missteps associated with imperfect information which have bedeviled every other central regulatory entity that have attempted to set prices administratively since Diocletian. I shouldn't fret. We are obviously smarter than every else in history who has attempted to do something similar in the past. We will finally get price controls to have the desired effects.
That's the ticket! An independent council. Now all of our problems are solved. All we need to figure out how the members of this council could remain independent (of what?), avoid issues of regulatory capture, and be able to avoid the missteps associated with imperfect information which have bedeviled every other central regulatory entity that have attempted to set prices administratively since Diocletian. I shouldn't fret. We are obviously smarter than every else in history who has attempted to do something similar in the past. We will finally get price controls to have the desired effects.
No matter what the discussion might start with, we always end with:
When the RBRVS system was pushed forward, I recall someone describing it as the worst of Harvard dressed up as the best of Chicago. Next, various central planning exercises have been dressed up as market driven efforts. Here we go again.
Value is now the buzzword. Everyone wants to purchase and deliver high-value products and services.
This is almost laughable if it were not so serious.
Interesting idea. Throw a bone to the docs. Give physicians immunity (partial?) from malpractice if they adopt tools and guidelines of care which likely have not been demonstrated to improve the quality of particular outcomes. I should not be so critical of the guidelines since they have yet been developed. That is what politics is all about. Alas, more experts.
Price signals are the most effective means to communicate dispersed knowledge to each other, in order to solve the economic calculation problem. When prices are administratively created they lack useful coordination information and send the wrong signals to economic players. For these authors, the path forward is paved with experts and planning. To entrust allocation of scarce resources in health care to true markets is inconceivable. This is the fatal conceit as described in Freidrich Hayek's book "The Fatal Conceit". We can only hope that they do not suffer from this conceit and really are smarter than those who have tried and failed before. I am not so optimistic.
Everyone (or at least almost everyone) agrees that we have a problem in health care. We are going broke because of costs. We have millions of uninsured. We have millions of under insured. We have problems with access to care, even among the ranks of the insured. We have problems with quality and safety. Have no fear, this elite group of very bright people can rebuild and rewire the house of medicine, even without having to turn the power off. There is a small problem, however. It appears as thought they haven't a clue as to how they can actually accomplish this these tasks. Take for example their first charge:
I couldn't agree more that the current system is a mess and not sustainable, but let me try to understand this alternative. Who would negotiate and with whom would they negotiate if whatever deal they struck would be binding on other parties with whom they did not negotiate? Negotiation requires effort and information on costs, local factors, alternatives, and countless other details. Which entity would invest in amassing this information if there are no particular advantages."PROMOTE PAYMENT RATES WITHIN GLOBAL TARGETS
Under our current fragmented payment system, providers can shift costs from public payers to private payers and from large insurers to small insurers.5 Since each provider negotiates payment rates with multiple insurers, administrative costs are excessive. Moreover, continued consolidation of market power among providers will increase prices over time.6 For all these reasons, the current system is not sustainable.Under a model of self-regulation, public and private payers would negotiate payment rates with providers, and these rates would be binding on all payers and providers in a state. Providers could still offer rates below the negotiated rates."
But there is more...
"The privately negotiated rates would have to adhere to a global spending target for both public and private payers in the state. After a transition, this target should limit growth in health spending per capita to the average growth in wages, which would combat wage stagnation and resonate with the public. We recommend that an independent council composed of providers, payers, businesses, consumers, and economists set and enforce the spending target."
No matter what the discussion might start with, we always end with:
Again, I will not defend the present fee for service system, but it is not a fee for service system alone which creates the current nightmare. It is the FFS system coupled with a third party payer which allows for providers to deliver and patients to receive often near worthless services without rapid feedback as to the cost. The global payment system will have its challenges and it is being foisted upon us on the assumption that it simply cannot be worse than what be presently have. It will succeed in its major goal by successfully stinting on care and not raising too much of a public protest."ACCELERATE USE OF ALTERNATIVES TO FEE-FOR-SERVICE PAYMENT
Fee-for-service payment encourages wasteful use of high-cost tests and procedures. Instead of paying a fee for each service, payers could pay a fixed amount to physicians and hospitals for a bundle of services (bundled payments) or for all the care that a patient needs (global payments)."
When the RBRVS system was pushed forward, I recall someone describing it as the worst of Harvard dressed up as the best of Chicago. Next, various central planning exercises have been dressed up as market driven efforts. Here we go again.
I am all for competitive bidding for things that are truly commodities but what is a commodity? By what criteria will the bids be awarded? I can only guess. Do we need to buy American? What about union vs non-union? Environmentally friendly? Again we see the experts. Who is on the panels of experts? By what process will they be selected? This will be done within the political world by a political process with a political outcome. Success will be ultimately measured by the garnering of votes."USE COMPETITIVE BIDDING FOR ALL COMMODITIES
Evidence suggests that prices for many products, such as medical equipment and devices, are excessive.9 Instead of the government setting prices, market forces should be used to allow manufacturers and suppliers to compete to offer the lowest price......We suggest that Medicare immediately expand the current program nationwide. As soon as possible, Medicare should extend competitive bidding to medical devices, laboratory tests, radiologic diagnostic services, and all other commodities.12 Medicare's competitively bid prices would then be extended to all federal health programs.13 To oversee the process, we recommend that Medicare establish a panel of business and academic experts."
Value is now the buzzword. Everyone wants to purchase and deliver high-value products and services.
It is like Lake Wobegon where all the children are above average. Since value will be defined as high quality and low cost, and no one really can measure quality, it is all about cost. I agree that price transparency is essential and I have nothing against tiers in pricing, as long as the information transmitted by differential pricing contains useful information. Which leads us to the next recommendation.."REQUIRE EXCHANGES TO OFFER TIERED PRODUCTS
The market dominance of select providers often drives substantial price variation.14 To address this problem, insurers can offer tiered plans. These insurance products designate a high-value tier of providers with high quality and low costs and reduce cost sharing for patients who obtain services from these providers........Transparency and consumer education are essential.17 Quality and cost measures must be standardized and publicly disclosed, and standards must be set for how these measures are used to create tiers. Whenever possible, quality measures should use data from all payers. Finally, in contracts between insurers and providers, clauses that inhibit tiered products must be prohibited."
Note all of this in contingent upon the existence of reliable quality reporting systems which do not yet exist! Also remember that these exchanges are not about the purchase of actual health care services, they are involved in the purchase of insurance. They will be charged with the task of driving prices down first and examining their effect on quality later, if an when the tools become available to do so.REQUIRE ALL EXCHANGES TO BE ACTIVE PURCHASERS
If exchanges passively offer any insurance product that meets minimal standards, an important opportunity will be lost. As soon as reliable quality-reporting systems exist and exchanges achieve adequate scale, it is critical that federal and state exchanges engage in active purchasing — leveraging their bargaining power to secure the best premium rates and promote reforms in payment and delivery systems.
This is almost laughable if it were not so serious.
Yes there are gains to be had from uniform credentialing, common information exchanges, and streamlined eligibility processes. But they must be joking! The informatics infrastructure to implement all the above will make the $360 billion in administrative costs look like chump change. This will require huge investments and complete re-engineering of workflows in millions of separate offices. They miss the obvious here. The inclusion of insurance into more and more transactions which should be be insured is the driver of the ballooning administrative costs. And yet another task force of experts working within the political realm.SIMPLIFY ADMINISTRATIVE SYSTEMS FOR ALL PAYERS AND PROVIDERS
The United States spends nearly $360 billion a year on administrative costs,19 accounting for 14% of excessive health spending.20 Section 1104 of the ACA requires uniform standards and operating rules for electronic transactions between health plans and providers.11 Although plans must comply with these standards and rules, the law does not require providers to exchange information electronically.First, we suggest that payers and providers electronically exchange eligibility, claims, and other administrative information as soon as possible. Second, public and private payers and providers should use a single, standardized physician credentialing system. Currently, physicians must submit their credentials to multiple payers and hospitals. Third, payers should provide monthly explanation-of-benefits statements electronically but allow patients to opt for paper statements. Fourth, electronic health records should integrate clinical and administrative functions — such as billing, prior authorization, and payments — over the next 5 years. For instance, ordering a clinical service for a patient could automatically bill the payer in one step.Most important, we recommend that a task force consisting of payers, providers, and vendors set binding compliance targets, monitor use rates, and have broad authority to implement additional measures to achieve systemwide savings of $30 billion a year.21
REQUIRE FULL TRANSPARENCY OF PRICESSounds like a good idea. It may not be so easy to make sure we are comparing comparable services. Replacing a hip in a 90 year old may not be the same as replacing it in a 60 year old. I would take it one step further and allow for balance billing for providers who are not afraid to advertise they are more expensive.
Now for the absolute mother of wishes on the wish list...
Implementation of this would require a complete rethinking of licensing of professionals throughout health care. Don't get me wrong on this. The present licensing structure needs to change. There is no question that many of the tasks required to take care of patients can be delegated to workers without medical degrees. The authors propose to bribe states to loosen professional licensing standards. I cannot imagine where this will end up but wherever that might be the path will be littered with the debris of serious political battles. The winners may not include the public. When do the chiropractors get privileges to do colonoscopies as well as colon irrigations? When do the acupuncturists and message therapists get prescribing privileges. When do the optometrists get to do Lasik surgery? When will nurses run patient care teams in acute setting devoid of any physician oversight? When will they be directly supervising physicians?MAKE BETTER USE OF NONPHYSICIAN PROVIDERS
Restrictive state scope-of-practice laws prevent nonphysician providers from practicing to the full extent of their training. ........
We recommend that the federal government provide bonus payments to states that meet scope-of-practice standards delineated by the Institute of Medicine.
Except for when we are dealing with ACOs. In that case self referral is exempted. This is an unnecessary level of complexity. Everyone else in the world refers to themselves. The major difference is when this happens, people sharply examine the transaction since they personally pay the bill. Give patients more skin in the game and the Stark Law becomes irrelevant.EXPAND THE MEDICARE BAN ON PHYSICIAN SELF-REFERRALS
Many studies show that when physicians self-refer patients to facilities in which they have a financial interest, especially for imaging and pathology services, they drive up costs and may adversely affect the quality of care.24,25
Sure, make federal employees play by the same rules as the rest of us. Throw Congress in there as well. And make the Feds use the same accounting rules that everyone else uses as well. I am a reasonable guy.LEVERAGE THE FEDERAL EMPLOYEES PROGRAM TO DRIVE REFORM
The Federal Employees Health Benefits Program (FEHBP) provides private health insurance to 8 million federal employees and their families.
REDUCE THE COSTS OF DEFENSIVE MEDICINE
More than 75% of physicians — and virtually all physicians in high-risk specialties — face a malpractice claim over the course of their career.28 .......
A more promising strategy would provide a so-called safe harbor, in which physicians would be presumed to have no liability if they used qualified health-information-technology systems and adhered to evidence-based clinical practice guidelines that did not reflect defensive medicine. Physicians could use clinical-decision support systems that incorporate these guidelines.
Under such a system, the physician could use the safe harbor as an affirmative defense at an early stage in the litigation and could introduce guidelines into evidence to avoid a courtroom battle of the experts. The patient could still present evidence that the guidelines were not applicable to the particular situation, and the judge would still determine their applicability.
It is critical to develop guidelines with credibility. A promising step is an initiative called Choosing Wisely, in which leading physician groups released guidelines on 45 common tests and procedures that might be overused or unnecessary.32 Given the important role of guidelines, physicians who participate in developing them must be free from financial conflicts of interest.
CONCLUSIONS
These are the types of large-scale solutions that are necessary to contain health costs. Although many in the health industry perceive that it is not in their interest to contain national health spending, it is a fact that what cannot continue will not continue.
Americans therefore face a choice. Payers could simply shift costs to individuals. As those costs become more and more unaffordable, people would severely restrict their consumption of health care and might forgo necessary care. Alternatively, governments could impose deep cuts in provider payments unrelated to value or the quality of care. Without an alternative innovative strategy, these options will become the default. They are not in the long-term interests of patients, employers, states, insurers, or providers.
Subscribe to:
Posts (Atom)